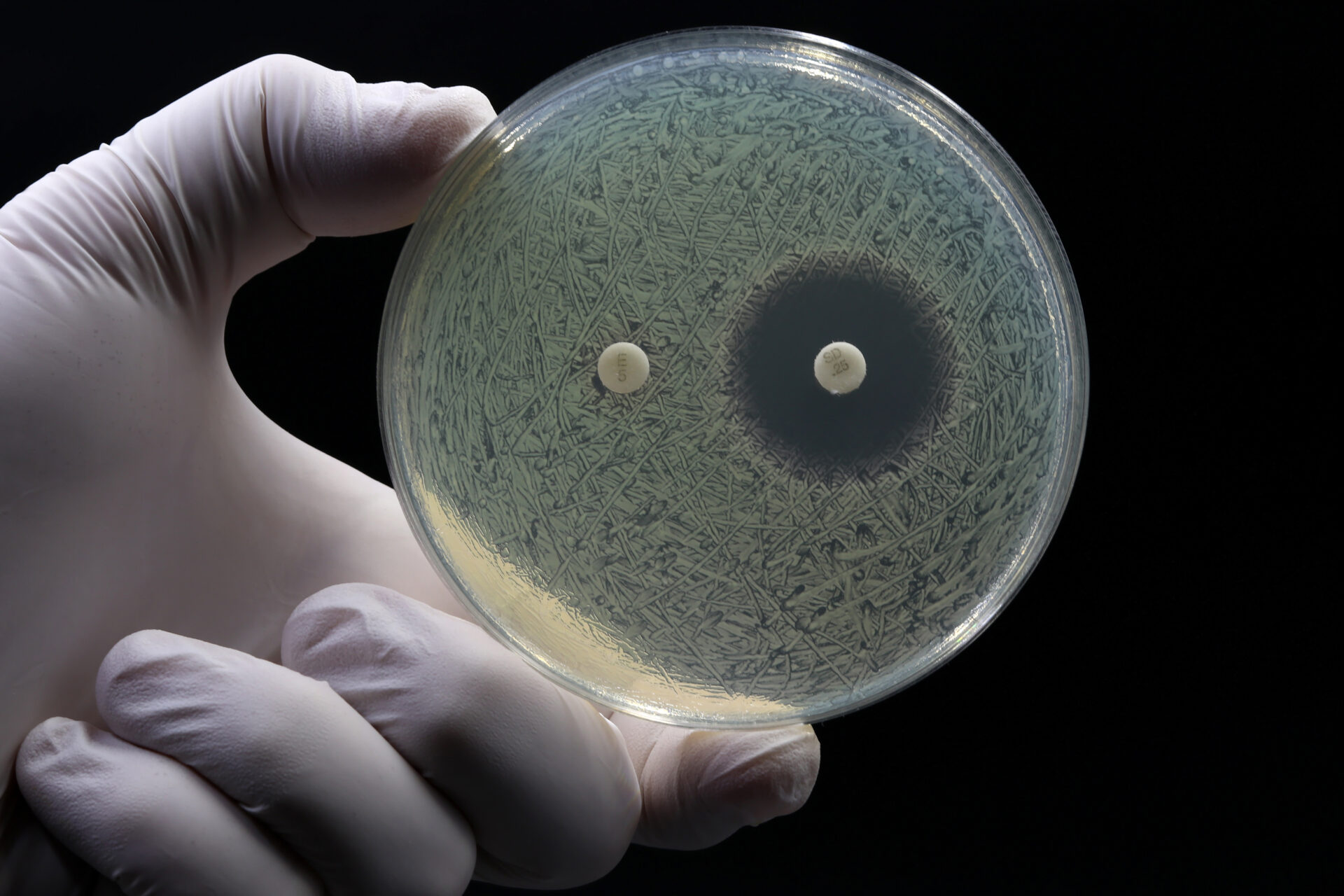
Clovibactin seems to be an impressive new antibiotic, at least per current research results–\As we move through the wake of the official COVID-19 pandemic, there’s a great deal of focus on new antiviral and antibiotic treatments in various forms. This interest has, in turn, spurred on a new round of research, funding, and exploration into new potential approaches to treating multiple infections and diseases. While this isn’t unusual in the world of medical research, this particular incarnation of it has led to some exciting discoveries. Clovibactin is a new antibiotic that–while still in its early phases of research and use–does seem to offer some powerful possibilities for treating bacterial infections while not fostering resistant strains. Clovibactin isn’t available as a prescription medication yet, but if the results it has produced thus far remain consistent, we may see it become available quickly.
What is Clovibactin?
Clovibactin is derived from soil bacteria Eleftheria terrea sp carolina, which was first isolated in soil samples collected in the sands of North Carolina. Soil bacteria are often the source of new antibiotic treatments. Commonly used antibiotics that were developed in the 1950s and 60s such as streptomycin, vancomycin, or tetracycline, use soil bacteria. Utilizing recent developments in screening and culturing techniques, NovoBiotic Pharmaceuticals and Northeastern University research microbiologist Kim Lewis were able to isolate Clovibactin from E. terrea sp carolina.
How does Clovibactin Work?
Clovibactin’s efficacy against both bacteria and antibiotic resistance is a function of the mechanism by which it works. Clovibactin is derived from Teixcobactin, a secondary metabolite of the E. terrea bacteria, which resembles a peptide in form and function. Teixobactin attacks bacteria by inhibiting cell wall synthesis, and it does this by wrapping tightly around the bacteria in question and bonding with lipid II, a precursor to the cell wall’s formation. This, in turn, destroys the integrity of the cell wall and serves as the killing function for the resulting antibiotics like Clovibactin.
The current research indicates that Clovibactin is effective against all gram-positive bacteria thus far tested, including bacteria that are notoriously difficult to treat, such as Staphylococcus aureus, Enterococci, and Mycobacterium tuberculosis with Clostridium difficile and Bacillus anthracis proving especially vulnerable.
The Limits of Clovibactin
Clovibactin seems to be an impressive new antibiotic, at least per current research results–no resistant strains have been identified in bacterial samples subjected to testing. However, this is not to say that prolonged testing or extended and widespread “real world” use would not create such strains; time will tell.
Another limit is biological: Clovibactin’s killing functions are ineffective against gram-negative bacteria, which have an outer membrane that successfully resists its envelopment effect. As with all new medications, Clovibactin has its limits, and doubtless, further questions will arise as testing and research continue.
The Future of Clovibactin
So where does that leave us, the end-users and patients who may benefit from this new medication? It may be some time before Clovibactin clears the necessary regulatory hurdles to become available to physicians and hospitals. Still, it is a promising new drug in and of itself and in terms of what it represents. Clovibactin origins–uncultured bacteria collected in the wild–suggest that further new medications with new mechanisms of action may be out there yet undiscovered. With antibiotic-resistant illnesses a growing concern worldwide, this new source of potential treatments offers opportunities and hope for better care and outcomes.
